“So we’re gonna go ahead and go live… Hey! How we doing?” announces David Stoecker via a Facebook Live session on February 24. There are about a dozen monitoring the feed from a digital device, while a handful of us watch Stoecker in person from inside the Springfield Recovery Community Center.
“Today what we’re gonna talk about is Narcan,” says Stoecker, his camera phone sitting at an angle on the table to capture his face. “Narcan is something that instantly reverses an overdose.”
He’s also the executive director of Better Life in Recovery, a nonprofit that helps those struggling with substance abuse and mental health issues through community service and education events; including this presentation on Naloxone, also known by the brand name Narcan.
“So we’re looking at a huge influx of heroin that’s coming into our community,” he tells the live stream’s followers.
Last August, after Missouri lawmakers passed HB 1568, Naloxone became legal for citizens to purchase as a third-party prescription under physician protocol. In other words, it does not require a doctor’s prescription. Now, any individual has the opportunity to administer the antidote to someone suffering from an opioid-induced drug overdose.
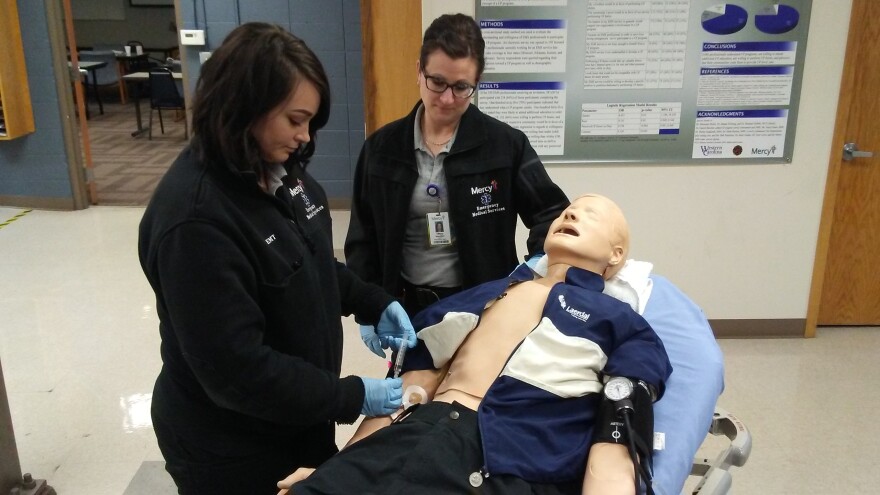
For decades, Naloxone has been a common tool for emergency medical services (EMS) personnel.
“This is .4 milligrams and 1 CC [Cubic centimeter] so you would pull up how much? 1 CC – perfect. And give it an IV push,” explains Luke Walker, paramedic program coordinator with Mercy Springfield, to his interns.
He's directing interns to administer Naloxone. Using a dummy lying in a stretcher as their subject, the students show how this drug overdose antidote can be injected intravenously, shot into a person’s muscle, or sprayed up a victim’s nose - that’s the most affordable version of the product for citizens.
“Once you push it [nose injector] hard, it just atomizes that medication up into that really vascular tissue and allows it to absorb good,” says Walker.
There were 1,066 drug overdose deaths in Missouri in 2015, the latest year data is available. The figure is one fewer than the year before. Compared to five years ago, and the state has experienced a slight uptick in such deaths. These days, lethal and non-lethal overdose cases are a rather common occurrence for local officials, says Bob Patterson, executive EMS director for Mercy Health System.
“So specifically to drug overdoses where we suspect a narcotic such as heroin we’re seeing one or two a day is our current average across our system,” says Patterson.
The hospital covers roughly half the city and county – with CoxHealth responsible for much of the rest. Combine their numbers, and emergency crews in Springfield/Greene County respond to roughly 15 overdose calls a week, with a majority of those opioid-related.
In fact, as Patterson was escorting me from the paramedic training room to his office for this interview, he stops an EMS driver that had just returned from a call.

“Just curious was that a heroin overdose? Patterson asks. “Yes it was,” the driver responds.
The Centers for Disease Control and Prevention says more than six out of every 10 drug overdose deaths in the nation are attributed to prescription or illicit opioids. The numbers are on par with Greene County, whose Medical Examiner office tells KSMU that in 2015, 63 percent of overdose deaths were linked to opioids.
“From our understanding, from what our law enforcement partners tell us is that it’s much more affordable and easy to get. So that’s why we’re starting to see those increases and rise in issues in utilization” says Patterson.
Patterson says drivers are generally equipped with enough Naloxone to cover two calls each departure, should they get another call before refilling supplies back at the station.
Drug seizures can be an indication of actual drug use. A recent analysis by the Springfield News-Leader shows more citizens were doing methamphetamine, heroin and ecstasy in 2015 than the year before. 327 grams of heroin, an opiate, were seized in 2015. That’s more than in the previous three years combined.
Those statistics, and the ones seen statewide, is in part why Missouri lawmakers passed the law making Naloxone available third-party, and why David Stoecker is conducting this education session.
“You’re gonna hear there’s a huge influx of fentanyl and carfentanil. It’s another reason we’re losing a lot of lives, is fentanyl is being used to cut heroin with. And because of that people are getting something that’s stronger than they thought it was.”
Stoecker displays the Naloxone products available to citizens. The first is the more common and less expensive nasal spray. The latter being the auto-injector, which can be easily administered into a leg muscle.

“If I were to go to CVS and get this without a prescription right now I think it’s gonna cost me about $144 for two of these. If I were to buy two of these it’s gonna cost me $4,400.”
“The silver lining of this is they’re available under most insurance,” says Steve Lynch, a Republican state representative from Waynesville, who sponsored the Naloxone bill.
He also sponsored the 2014 bill which is now law that allows first responders like police and fire rescue personnel to carry Naloxone. Neither Springfield’s police nor fire departments carry the antidote.
Lynch says it’s tough to judge the effectiveness of the Naloxone law to date – there’s no tracking of product sales or statistics on how much it’s been used since the law took effect. But he notes that more protections are needed so that people using the product feel safe to contact emergency personnel. That’s because while some 80 percent of drug overdoses occur with someone else around, more often than not the victim is found alone.
“Because of the fear that if they call they’re [the bystander] gonna get arrested, they don’t call. So they’re actually just leaving them [overdose victim] there… and of course people are dying that could possibly be saved.”
Another concern, says Lynch, is some overdose cases may require more than one dose of Naloxone. And carriers may not have another to give.
“So they need to call emergency services even if they administer a dose of it. Because it’ll bring the person right out of it, but in an half hour – depending on how much heroin is in their system – it’ll go right back to causing them to suffocate again – which is what it does – and they’ll need another dose. And they may not have any more there.”

This year, Lynch has filed HB 294, known as the Good Samaritan Law, which would protect drug victims and bystanders from arrest if the paraphernalia found on scene is of a “personal use” amount. In other words, there are not enough drugs that would indicate intent to distribute.
Lynch notes that while he’s always believed if you do the crime you do the time, at some point drug abuse changed ”from a crime issue to a life issue.”
“The disease of addiction is horrible stuff, it comes with a horrible stigma that people think they can just get off it if they want to. It doesn’t work that way,” Lynch says.
Back inside the Springfield Recovery Community Center, David Stoecker is offering tips during his Facebook Live session on ways to help overdose victims without the product.
“Even if you don’t have Narcan, rescue breathe, call 9-11, keep breathing every six seconds until the ambulance gets there,” says Stoecker.
These life-sustaining strategies, he hopes, can buy enough time for the abuser to where they eventually seek assistance and get on the road to recovery.
Follow Scott Harvey on Twitter: @scottksmu


