One out of every nine babies are born prematurely in the United States. Such births have risen by more than 36 percent over the last two decades, according to the March of Dimes (MOD). Yet experts are unsure why. As part of Prematurity Awareness Month, the MOD recently announced that the third of five facilities dedicated to prematurity research will be in Missouri. KSMU’s Theresa Bettmann has more on what this means for future parents.
Premature birth is the leading cause of death in newborns, according to the March of Dimes (MOD). Each year, the agency puts out a premature birth report card ranking each state. Sharyn Dawson is the director for MOD Ozarks Division.
“About 14,000 babies are born a year in the Ozarks division. And of that just over ten percent of them are born premature. So our grade of a “C” is because we are higher than the national average right here,” says Dawson
The state’s poor ranking is one reason why Dawson and other officials feel the new research facility, at Washington University in St. Louis, is critical for Missourians. Babies born prematurely can experience lifelong health consequences like blindness, hearing loss, asthma, cerebral palsy and other chronic conditions.
If premature births could be prevented in the Ozarks, says Dawson, it would allow a financial savings of $71 million in insurance premiums, medical costs and other related expenses. She adds there is no price that can be placed on the emotional toll it has on families.
Danielle Wagner and her husband Steve understand the emotional roller coaster all too well.
“We got pregnant and went in for our first ultrasound where they proceeded to tell us we were not having one baby, but we were having triplets,” Wagner says.
Not long after the couple learned they were actually having quadruplets. Wagner knew she was not likely to make it to full term and could be at high risk. But that did not prepare her and her husband for what happened next.
The babies were born at 24 weeks, each weighing little over a pound.
“They assembled roughly 32 people in the operating room for my deliver within an hour,” says Wagner.
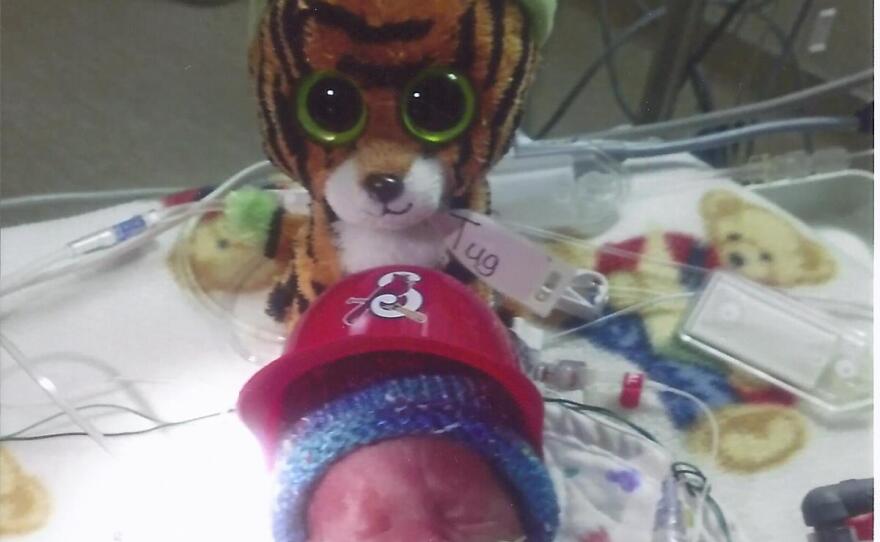
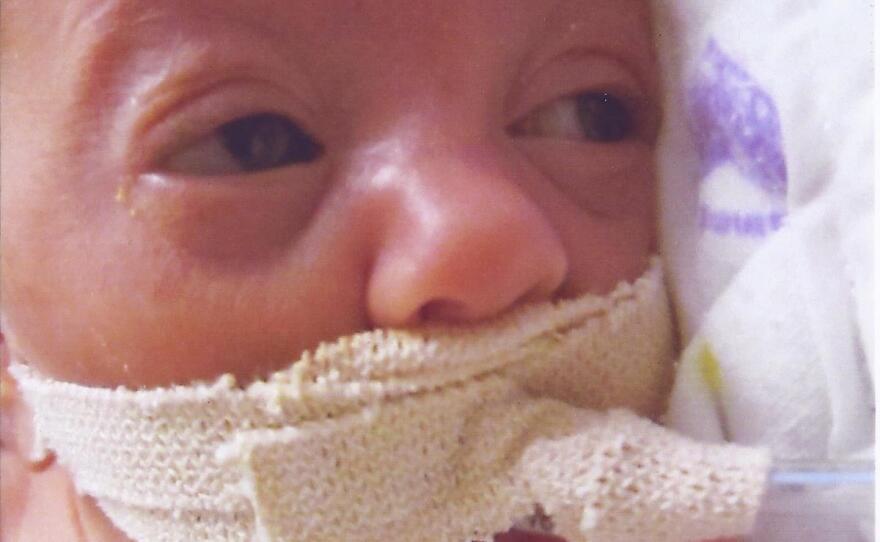
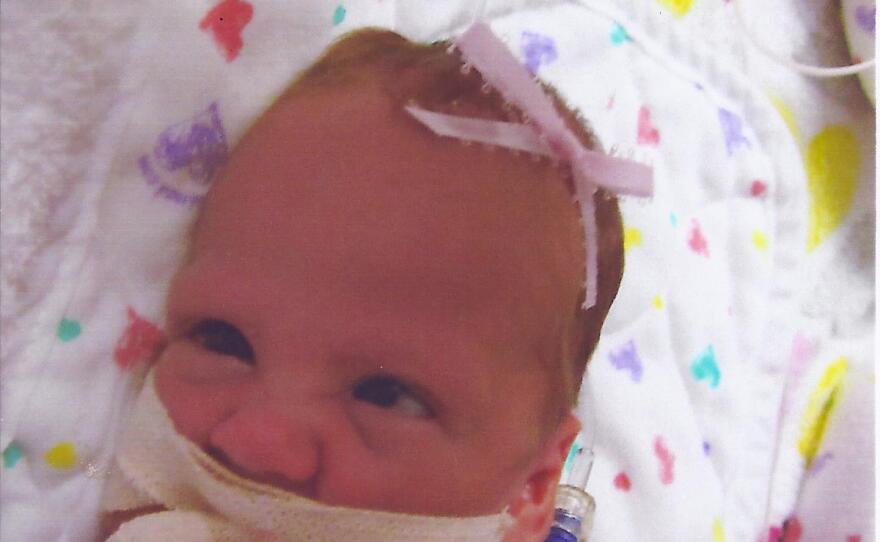
Briar, Hadley, Grant and Rowan were around 11 inches long with feet the size of paperclips. Their little arms were so small that blood pressure cuffs were the size of Band-Aids. Wagner shares that the next few months was an emotional whirlwind of ups and downs.
After two months at Mercy Springfield’s neonatal intensive care unit (NICU), Rowan passed away.
“At a point you have to hold onto the positive in this situation, and it may not look there is any positive. But you have to find something because you have to get out of bed and you have to show up and you have to be by your baby’s side every step of the way and it’s not going to be easy,” explains Wagner.
Briar, Hadley, Grant would remain at the NICU two more months, with mom and dad virtually living in the nearby Ronald McDonald house to be close by.
The triplets are now 15 months old and doing well, says Wagner. Grant is being monitored for vision complications as a result of prematurity. Wagner says they are where they are today because of the ongoing support they received beginning with the Neonatal Intensive Care Unit (NICU).

Dr. Edward Stevens has been a neonatologist for 30 years.
“I did a rotation through the neonatal unit I think my first month as a pediatric resident, and that was all I wanted to do after that,” Stevens shares.
Stevens says that while it was intensity and excitement which first drew him into the field, it was also emotionally challenging. He says he has seen remarkable transformations over the years as a result of research.
“Neonatology is really one of the fields of medicine that is literally in its infancy and making improvements by leaps and bounds. When I first started a 25-week preemie had a 10 percent chance of surviving. Now that survival is closer to 80 percent. We look at ourselves and ask ‘what went wrong’ now when we lose a tiny preemie,” says Stevens.
Preventing birth defects, vaccine development and learning more about the causes of prematurity are areas for more exploration. Research has provided treatments like steroids to be given prior to delivery to help with the baby’s lung development, as well as many other medications.
“Some examples are surfactant which is a medication used— some call it a miracle drug for preemies—it’s a substance that they are missing from their lungs. When it is instilled it has a dramatic impact on how well they can breathe,” says Stevens.
Stevens says the NICU has an average of 30 babies at any given time, and is in the process of expanding to provide for up to 50. He says one of the most rewarding things about his job is to see children and families each year at the preemie reunion.
Wagner shares that her family’s overall experience has been nothing short of a roller coaster ride. The bright spot, she says, centers around the lifelong relationships they’ve developed. Something she will never forget.
The research facility in St. Louis is part of a $75 million project by the March of Dimes in placing five prematurity centers across the U.S. The St. Louis location at Washington University launched November 10th. The first research complex was established in Ohio, and the second was in California. The fourth location at the University of Pennsylvania was announced on Monday and the fifth location has yet to be determined.